Reusing protective equipment could safeguard against the risk of future shortages as well as reducing its environmental impact. With funding from the MAS Foundation, a group of researchers is close to finalising a PPE disinfection and reuse solution.
For frontline health workers dealing with COVID-19 patients, personal protective equipment (PPE) is essential. But at various points over the past year, PPE has been in short supply, putting workers at risk and posing challenges for patient care.
Since mid-2020, a group of researchers has been collaborating on a way of disinfecting PPE for potential reuse. Supported by funding from the MAS Foundation and support from MBIE’s COVID-19 Innovation Acceleration Fund, the project has been led by Dr Yvonne Anderson – senior lecturer in population child health and paediatrics at the University of Auckland. Yvonne and her team are working alongside the Universities of Otago and Canterbury and New Zealand company UV Solutionz.
Yvonne says the project is focused on improving New Zealand’s response to future pandemics, and they hope to have a proof of concept for potential rollout in the next few months.
-

“If we can create a process that healthcare workers and their patients can trust, then we’ll have a vital insurance policy against running out of this essential equipment in the future.”
Dr Yvonne Anderson (Photo credit: L’Oréal)
“While we’re mainly focused on protecting healthcare and other frontline workers against the virus, disinfecting and reusing this equipment may help the health system reduce the amount of medical waste it produces.”
Securing the availability of PPE
Yvonne is a frontline healthcare worker herself, giving her first-hand knowledge of the volume of PPE required to deal with the pandemic.
She says it was clear from the early days of the pandemic that New Zealand was facing PPE shortages if we experienced similar numbers of COVID-19 cases as had been seen overseas.
“We began to look at ways that we could shore up the supply of PPE for the frontline, and part of that puzzle was looking at whether we could disinfect it safely for reuse. To put it in context, if we can develop an effective disinfection protocol, we could potentially increase the available supply of N95 face masks alone by 400%.”
Yvonne says the research team took a ‘whole of PPE approach’, trialling the disinfection process on gowns, N95 masks, surgical masks, face shields and eyewear.
“Our first step involved testing our methods of disinfection. We have been studying heat and UV disinfection methods against SARS-CoV-2 – the virus that causes COVID-19.
“We’re working with Professor Miguel Quiñones-Mateu and his team in Dunedin at the University of Otago. They have the virus in a highly contained lab, and Professor Quiñones-Mateu is running tests to see if our methods inactivate the virus on items of PPE,” Yvonne says.

Professor Miguel Quiñones-Mateu and his team
Creating a prototype
Once the research team has established that their methods work, they intend to undertake materials testing with Associate Professor Mark Staiger at the University of Canterbury, where Mark and his team will test the PPE to ensure that it hasn’t been compromised by the disinfection process.
After ensuring the process is working safely, the team are building a prototype of a mobile disinfection solution in Taranaki, under the supervision of Geoff Ray from GWR United Services Ltd.
Yvonne says, theoretically the prototype could be rapidly implemented across the country or further afield if necessary.
Running in parallel with the scientific research, the team have been working hard to prioritise frontline worker voices.
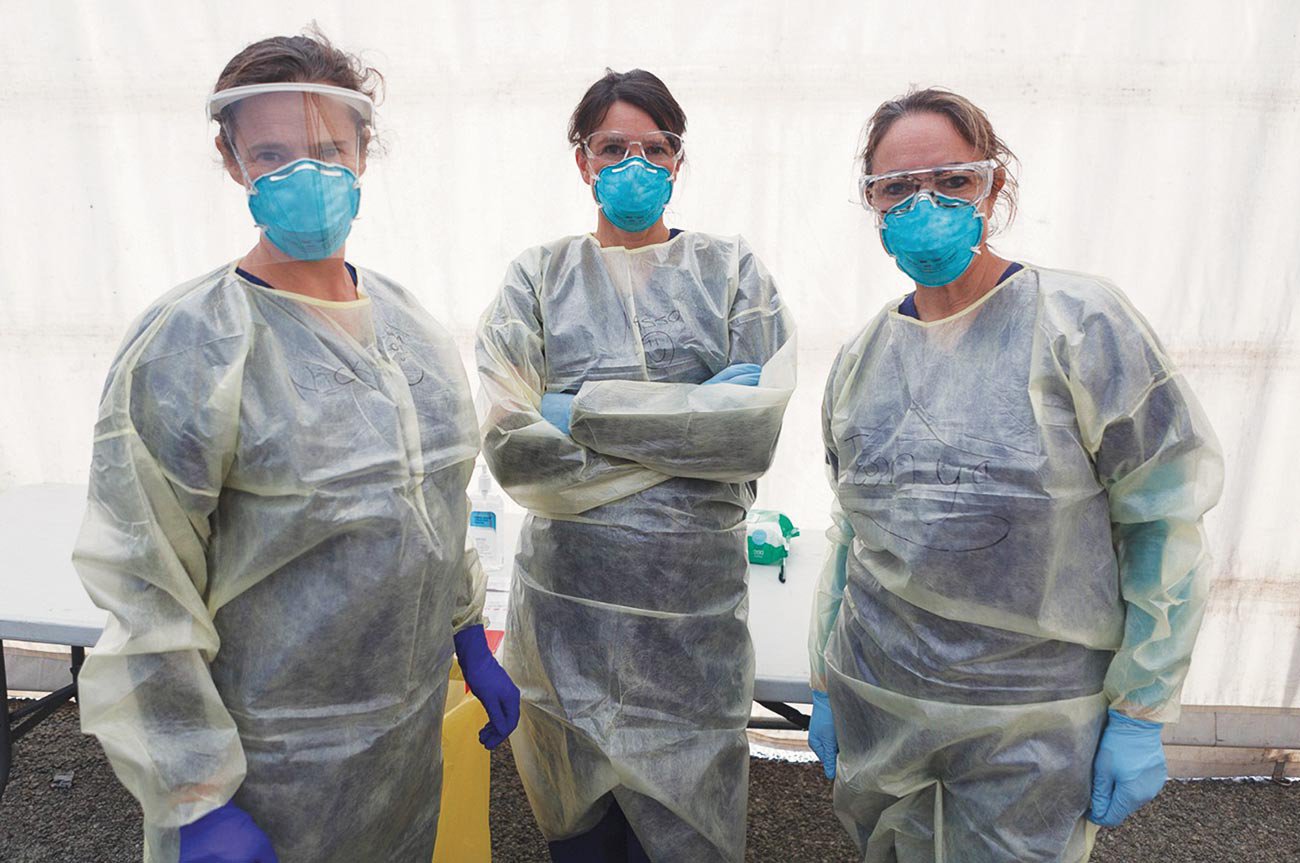
Frontline healthcare workers wearing PPE. Credit Pharmacy Today
“We were humbled to receive over 1,500 responses to our end-user acceptability survey, where many also shared their experiences of PPE use during wave one. These findings will stand alongside any disinfection solution we achieve as it is paramount that we receive feedback from potential end users.”
The final stage of the research will be ensuring that their methods are tested against other key bacteria and viruses that may be present on PPE in the healthcare environment.
The importance of support
Yvonne says the funding provided by the MAS Foundation and MBIE’s COVID-19 Innovation Acceleration Fund has been crucial to this research project.
“The MAS Foundation funding was fantastic because it meant we’ve been able to employ extra support for the team and provide ongoing career opportunities for emerging researchers."
Dr Yvonne Anderson
“What has been great with working with the MAS Foundation is their flexible approach and high trust environment with researchers. They have been really committed to building a relationship with the research team and ensuring they can support us in delivering high-quality outputs.”
Know someone who might enjoy this?
Greater good
See all-
March 2021
Candles for a cause
-
March 2021
Helping Kiwi babies thrive
-
March 2021
Creating a Deaf-inclusive Aotearoa
-
July 2021
Rebuilding after the Lake Ōhau fire



